29
Nov
Study Finds Novel Relationship Between Shingles and Pesticide Exposure
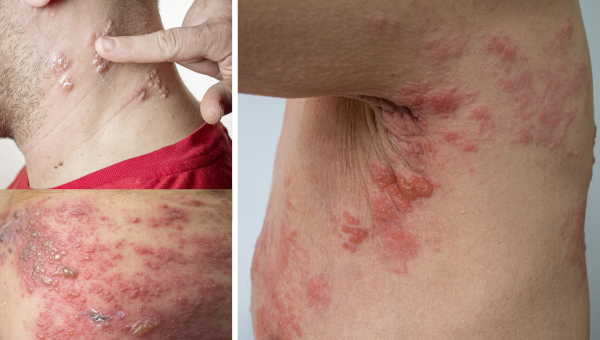
(Beyond Pesticides, November 29, 2023) A study published in Environment International finds high pesticide exposure incidence associated with shingles, a varicella-zoster virus (the same highly contagious virus that causes chickenpox) that reactivates in the body after having chicken pox. Shingles is a painful condition with a blistering rash that can lead to vision and hearing loss, brain and lung inflammation, and even death if not treated. Since shingles manifest decades after initial exposure, and the association is strongest among individuals already hospitalized for pesticide-related illnesses, researchers find the long-term/chronic effects most concerning. Although dermal pesticide exposure can cause a range of adverse reactions, including dermatitis, allergic sensitization, and cancer, any route of exposure can exacerbate dermal manifestations through immune system response, causing virus-based skin reactions like shingles.
People encounter toxic chemicals daily. However, frequent use of pesticides, including the use of everyday products like cleaning supplies, personal care products, agricultural chemicals, fabrics, non-stick cookware, and general airborne pollution, exacerbate chemical exposure risks. Dermal exposure is the most common pesticide exposure route, composing 95 percent of all pesticide exposure incidents, and is a significant concern for occupational (work-related) health.
The study notes, “[The] findings of elevated shingles risk associated with acute, clinically relevant pesticide exposures also highlights potential long-term costs of unintentional high-level pesticide exposures, especially those contributing to poisoning, which is a global problem in agricultural settings.”
Using 22,753 licensed private pesticide applicators of 66 years and older with more than 12 consecutive months of Medicare hospital and outpatient coverage between 1999 and 2016, researchers identified patients who experience at least one shingles incident. Additionally, researchers gathered information on whether patients received medical care for pesticide-related illnesses and if they encountered high pesticide exposure events (HPEE) and poisoning. The results find that 2,396 pesticide applicators were diagnosed with shingles during the 1996 to 2016 timeframe, with higher shingles rates among patients hospitalized for pesticide-related illness, pesticide poisoning, and HPEE. Thus, these initial findings suggest acute, high-level, and medically significant effects of pesticide exposure can increase shingles risk in individuals years to decades following exposure.
The skin responds to numerous external stimuli that can change its morphological (shape/structure), physiological (function), and histological (tissue) properties. Some responses to external stimuli are typical, including skin exposure to sunlight (UV-light) for tanning or water for wrinkling. However, exposure to excessive stimuli, including environmental contaminants, can propagate adverse, permanent changes to the skin. Just as excessive exposure to UV rays can cause skin discoloration and cancer, prolonged dermal contact with disinfectants can cause many adverse reactions, including skin discoloration and cancer. One of the most predominant routes of pesticide exposure is dermal, and most disinfectants are potential skin irritants and sensitizers (allergens), suggesting that direct skin contact with these toxic chemicals and the adoption of proper application protocol is critical.
Most pesticides cause some form of acute skin irritation. Although certain pesticides are less harmful to dermal contact than others, many chemicals cause irritant contact dermatitis (ICD) and allergic contact dermatitis (ACD). ICD is a nonimmune response that manifests into localized skin inflammation by directly damaging the skin following toxic agent exposure. ACD is an immune response to skin contact with a dermal allergen that an individual is already allergic (sensitized) to, causing nonlocalized skin inflammation and systemic bodily response. However, chronic, cumulative exposure to more mild chemical irritants can elicit a skin reaction. As skin cancer has increased significantly over the past 50 years, many appropriately point to the link between sun exposure and the development of the disease. However, this research indicates that contact exposure to herbicides may be affecting risk. The authors point to studies finding links between skin adsorption of pesticides and exposure to UV radiation, as well as research that finds sunscreen itself may facilitate skin adsorption of pesticide residue.
This study is the first to demonstrate the occurrence of shingles associated with pesticide exposure. However, this study is not the first to establish pesticides’ relationship with immune system disorders related to the skin. A Dutch study found that infants exposed to dioxins (a pesticide byproduct) and PCBs have a higher incidence of recurrent chicken pox, while, as mentioned, is linked to shingles.
Although this study notes that the mechanism involved in shingles incidence is not well understood, studies, including this one, suggest immune system suppression is the main culprit. The immune system offers the best defense against viral infection, as the virus stimulates an innate and adaptive immune response to expel viral particles from the body. Innate immune responses are the first line of defense against viral infections, activating myeloid immunocytes (cells that mediate immune responses against pathogens). These mediating cells create antibodies that the complement system (a network of proteins that eliminate pathogens) enhances. Therefore, review researchers speculate that immunocytes and the complement system can restrict viral infections. However, coronavirus infections can suppress/delay interferon (INF) protein synthesis responsible for defending against viral infections, causing a lapse in the innate defense system. Similarly, an adaptive immune response involves various immune cells and antibodies essential to protect against coronavirus infections. Still, injury to cells responsible for safeguarding against viral infections can induce more severe disease progression.
The global rate of shingles over recent decades is increasing despite vaccine availability. Therefore, there is an urgent need to evaluate the effect pesticide exposure and use have on disease health outcomes. Although some practices and products can prevent vital infections, the continued use of toxic pesticides increases disease risk factors. Beyond Pesticides tracks the most recent studies related to pesticide exposure through our Pesticide Induced Diseases Database (PIDD). This database supports the clear need for strategic action to shift away from pesticide dependency. For more information on the multiple harms of pesticides, see PIDD pages on body burdens (including skin reactions and diseases), immune system disorders, cancer, and other conditions.
Additionally, replacing pesticides with organic, nontoxic alternatives is crucial for safeguarding public health, particularly in communities vulnerable to pesticide toxicity. For more information on how organic is the right choice, see Beyond Pesticides’ webpage, Health Benefits of Organic Agriculture. Furthermore, visit Beyond Pesticides’ webpage on Disinfectants and Sanitizers and Least Toxic Control of Pests In the Home and Garden to learn more about safer, non-toxic pesticide alternatives.
All unattributed positions and opinions in this piece are those of Beyond Pesticides.
Source: Environment International











Thank you very much for your information! It helped me understand my 30 yr old sons shingle outbreak . He works for John Deere as a mechanic. His job sites are normally on the farm fields most likely full of pesticides.
January 7th, 2025 at 6:04 pmThis is very very important for him to know and which route he will go after this.
Thank you so much for sharing your son’s experiences Lea; please do not hesitate to reach our team for more information at [email protected]!
January 9th, 2025 at 11:31 ammy 6 yr old got exposed to pesticides exposure while playing at a park. An hr later I noticed red spots on my daughter neck cheeks . Her luch was the usual so the only think I can think of is the freshly cut grass and seeing the workers carry backpack with sprayer. i wish I would of know this before letting her play there. now 2 days layer the rash has spread to chest arms and face is more red. thankfully no fever and doesn’t inch. Do we know how long this might last? is there other factors to worry about?
March 2nd, 2025 at 2:40 pmHi Erica! Thanks for reaching out to our team and we are so sorry for what you are your daughter have experienced! A member of our staff will reach out to you directly over email with more information.
March 6th, 2025 at 4:28 pm